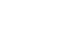
Bacterial prostatitis is a form of prostate inflammation caused by a bacterial infection. It accounts for about 10% of all prostatitis cases and differs from non-bacterial forms due to the possibility of identifying the responsible microorganism through culture tests.
Indice
Types of bacterial prostatitis
There are two main forms: acute bacterial prostatitis, characterized by sudden onset and severe systemic symptoms, and chronic bacterial prostatitis, a more subtle and persistent condition that represents the most common cause of recurrent urinary tract infections in men.
Acute bacterial prostatitis
Acute bacterial prostatitis is a urological emergency requiring rapid diagnosis and treatment. It typically presents with:
- High fever (often above 38.5°C) with chills and sweating
- Severe pain in the perineum, pelvic area, and back
- Severe urinary symptoms: urgency, frequency, dysuria, or even urinary retention
- General malaise, nausea, and marked weakness
On digital rectal examination, the prostate appears enlarged, warm, tense, and very tender. In severe cases, a prostatic abscess may form, a complication that requires surgical drainage.
Chronic bacterial prostatitis
Chronic bacterial prostatitis is characterized by recurrent urinary infections caused by the same bacterium persisting in the prostate. Symptoms are less acute but become chronic over time:
- Pelvic, perineal, or genital pain of varying intensity
- Moderate irritative or obstructive urinary symptoms
- Sexual dysfunction and pain during ejaculation
- Recurrent episodes of cystitis or urethritis
Between episodes, the patient may be asymptomatic or experience only mild discomfort. This feature makes diagnosis difficult and often leads to delays in treatment.
Responsible bacteria
The microorganisms most frequently involved include:
- Escherichia coli (responsible for 70% of cases)
- Klebsiella pneumoniae
- Pseudomonas aeruginosa
- Enterococcus faecalis
- Proteus mirabilis
Microorganisms such as Chlamydia trachomatis, Mycoplasma genitalium, and Ureaplasma urealyticum may also be involved, especially in sexually active young men.
How is bacterial prostatitis diagnosed?
Diagnosis is based on clinical symptoms, digital rectal examination, and laboratory investigations. The main diagnostic tests include:
Four-glass test (Meares–Stamey): compares bacterial cultures and leukocytes in samples of initial urine, midstream urine, prostatic secretion after massage, and first urine after massage
Urine culture and antibiogram: essential for identifying the bacterium and selecting the most effective antibiotic
PSA (prostate-specific antigen): may be significantly elevated during the acute phase and normalize after recovery
Transrectal prostate ultrasound: useful to exclude abscesses and evaluate gland size
Treatment of bacterial prostatitis
Treatment includes:
- antibiotic therapy guided by antibiogram, lasting at least 3–6 weeks
- anti-inflammatory drugs
- phytotherapy based on rye pollen
Prognosis and risk of recurrence
Acute bacterial prostatitis, if treated promptly, generally has a good prognosis. The chronic form, however, tends to recur: clinical studies report recurrence rates of 20–40% even after adequate therapy.
To reduce the risk of recurrence, it is important to complete the prescribed antibiotic course, not discontinue therapy at the first signs of improvement, and undergo scheduled urological follow-ups.