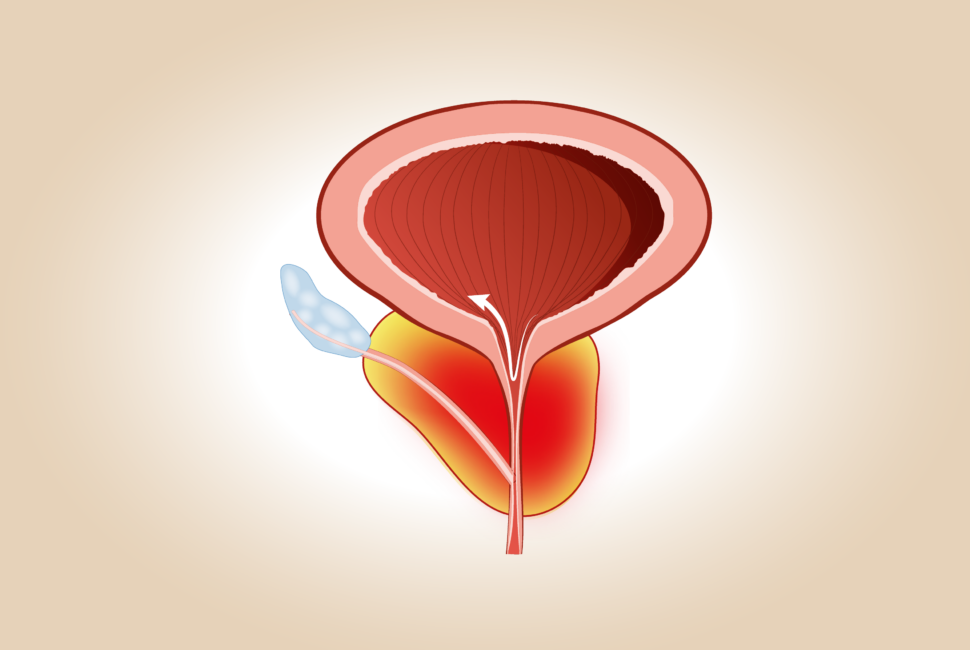
Chronic pelvic pain syndrome, also known as chronic non-bacterial prostatitis, is the most common form of prostatitis, accounting for 90% of all cases. It is defined by the presence of persistent pelvic pain for at least 3 months within the last 6 months, in the absence of a documented bacterial infection.
The term “non-bacterial” indicates that, despite negative bacterial cultures, the patient experiences painful and urinary symptoms that significantly impact quality of life. This makes it a complex and often frustrating syndrome for both patients and physicians.
Indice
Symptoms: how chronic pelvic pain syndrome presents
Symptoms include:
Pelvic and perineal pain
- Pain, pressure, or discomfort in the perineum (area between scrotum and anus)
- Suprapubic pain
- Testicular or penile pain (penalgia, orchialgia)
- Radiation to the lower back and lower limbs
Urinary symptoms
- Increased urinary urgency and frequency
- Difficulty initiating urination or weak stream
- Feeling of incomplete emptying
- Urethral burning
Sexual and ejaculatory symptoms
- Pain during or after ejaculation
- Erectile dysfunction
- Reduced sexual desire
- Hematospermia (blood in semen)
The psychological impact should not be underestimated. Anxiety, depression, sleep disorders, and social isolation are common in patients with chronic pelvic pain syndrome.
Diagnosis of chronic pelvic pain syndrome
Diagnosis is essentially one of exclusion. The goal is to rule out specific organic causes such as bacterial infections, tumors, stones, and anatomical abnormalities.
Diagnostic tools include:
- Urine culture and urinalysis (to exclude bacterial infections)
- Four-glass test or simplified Nickel test (pre- and post-massage)
- Transrectal and/or pelvic ultrasound
- Uroflowmetry with post-void residual
- Validated questionnaires such as the NIH Chronic Prostatitis Symptom Index, used to quantify symptom severity in three areas: pain, urinary symptoms, and quality of life
Treatments for chronic pelvic pain syndrome
There is no universally effective treatment. The best approach is multimodal and personalized:
- Anti-inflammatory drugs, useful for acute pain control
- Alpha-blockers to reduce urinary symptoms
- Pelvic floor physiotherapy
- Relaxation techniques and stress management
- Phytotherapy based on rye pollen